What Is Pilonidal Disease?
Pilonidal disease is a skin condition characterized by the formation of one or more abscesses or cysts in the fold between buttocks overlying the tailbone, also known as the sacrum.
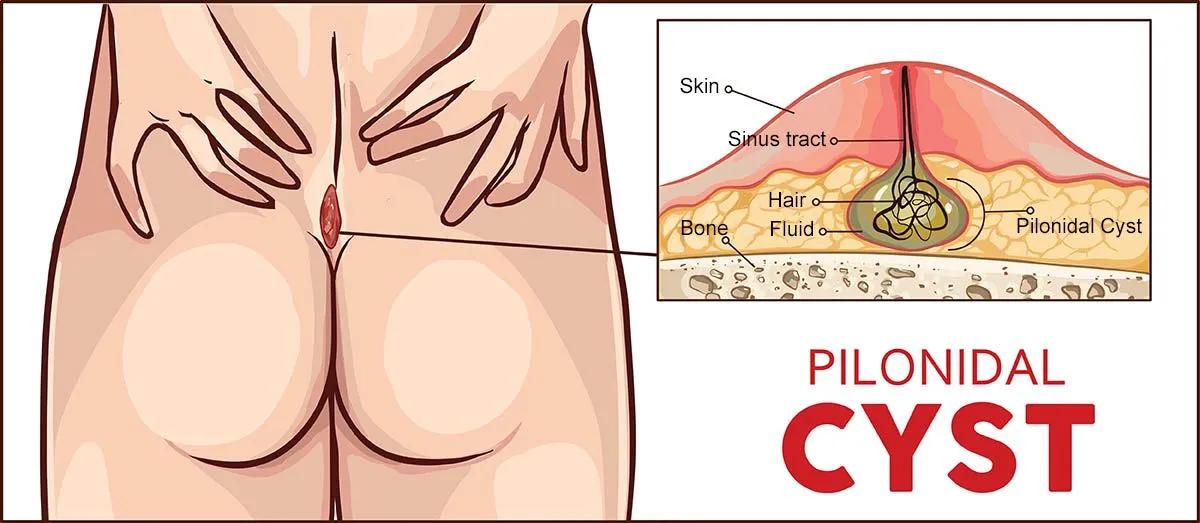
Understanding Pilonidal Disease
Pilonidal disease is an inflammatory condition affecting the skin and soft tissues overlying the sacrococcyx (tailbone). It is characterized by the formation of abscesses, cysts, or sinus tracts in the fold between the buttocks overlying the tailbone also known as the sacrum.
While the exact cause remains elusive, some of the leading theories attribute the cause to loose hair fragments being driven into expanded skin pores. Following entrapment of hair shafts, skin integrity becomes compromised and opportunistic bacterial infection occurs.
Risk Factors
Pilonidal disease is most prevalent in males between the ages of 15 and 40 years. Other risk factors include:
- Obesity
- Sedentary employment or lifestyle
- Increased body hair
- Family history of pilonidal disease
- Polycystic ovary disease (PCOS)
Presentation & Symptoms
Presentation of pilonidal disease varies from patient to patient. Most patients will describe some level of pain over their tailbone region and commonly attribute it to a potential trauma they may have sustained or to prolonged traveling.
An abscess, or a collection of pus beneath the skin, is what most often causes patients to seek medical attention at an emergency room or urgent care setting.
In less severe cases, patients will experience intermittent flare-ups of pain and swelling that spontaneously resolve, at times with the aid of some home remedies. Patients are also commonly prescribed antibiotics by their primary care providers or dermatology practitioners.
Approximately half of our patients will have undergone one or more unsuccessful surgeries elsewhere before learning about us.
Find Relief Today
Schedule Your
Consultation
Contact Pilonidal Fix today and let us help you leave your pain behind. Take the first step toward lasting relief with expert, compassionate care from Dr. Rafailov.
Call or Text
(973) 323-2400Hours
Mon–Thu 9–4, Fri 9:30–4